CQ ORTHOPAEDICS
Dr James Roche
Orthopaedic Surgeon
 |  |  |  |  |
|---|---|---|---|---|
 |  |  |
HIP REPLACEMENT SURGERY
You’ve Got Questions - I’ve Got Answers
TOTAL HIP REPLACEMENT
Hip replacement is one of the most successful procedures in modern medicine.
A hip joint is made of 2 components - a socket or cup that replaces the native acetabulum and a femoral stem that replaces the femoral head. These can either be fixed to host bone using cement or allowing the patient's bone to grow onto the surface of the implant. We use a variety of implants to suit each patient's anatomy and function profile.
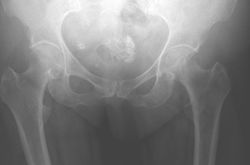
Arthritis
Most symptoms from the hip are due to osteoarthritis. Sometimes there will be a predisposing structural abnormality in the hip due to childhood conditions such as dysplasia of the hip, Perthes disease or slipped upper femoral epiphysis. Other causes of hip arthritis include inflammatory arthritis, infection or trauma.
Indications for surgery
Pain and loss of function are the major indications for hip replacement surgery. People have different pain thresholds so not everyone is ready for a hip replacement at the same stage of their disease.
Implant Survival
Joint replacement surgery was originally designed for relatively elderly and immobile patients. In these patients implant survival is greatest and exceeds 80% at 20 years for the implants used by Dr Roche. In younger patients the survivorship reduces primarily because of the increased activity and demand of more active patients. Advanced bearing surfaces have helped to mitigate this to a degree but the chance of needing additional revision surgery is certainly greater. However, hip replacement surgery can make an enormous difference to the quality of life in these patients. Dr Roche will discuss the timing of surgery with all patients to ensure it proceeds at the most appropriate time for each patient
APPROACHES FOR HIP REPLACEMENT
Posterior approach
This is the usual approach for most hip surgeons. It gives unimpeded access to both the femur and acetabulum, that allows the components to be placed with maximum accuracy. It can easily be extended for complex surgery, causes minimal damage to the muscles around the hip used for walking, and leaves a unobtrusive scar in the buttock. It is particularly suitable for minimally invasive surgery. The main drawback is an increased risk of dislocation for some surgeons.
Anterior and Lateral Approaches
These approaches are supposed to make the hip more stable but have a greater chance of damage of nerves and muscles around the hip. Often with the anterior approach the surgeon is limited to implant choice depending on the equipment used to help in the approach. We only use the lateral approach for hip fractures where the stability of the hip is more important than function.
Direct Superior Approach (DSA)
In the last 2 years this has become the default approach Dr Roche uses for primary hip replacement surgery and is gaining popularity in Australia. It requires special training and instruments but allows the use of standard, market-leading implants that have a long pedigree of success. It can also be used with either cemented or uncemented implants. It provides the excellent access to the acetabulum and femur provided by the posterior approach, but with a greater emphasis of tissue sparing. The scar is typically half the size of the posterior approach and is hidden beneath underwear. This approach results in less post-operative pain, earlier mobilisation and quicker return to function. Often this means an earlier discharge for those patients who wish to get home as soon as possible - many go home after just 2 nights in hospital and at this stage are walking independently with crutches and walking up and down stairs.
Dr Roche is one of the most experienced surgeons using this approach and is one of just four approved instructors in Australia. He teaches on a course for other Specialists wishing to learn this technique 3 or 4 times a year.
With the latest software this technique can now be performed with robotic surgery. Dr Roche will be the only surgeon in the region able to combine robotic surgery with the minimally invasive and muscle sparing Direct Superior Approach to give his patients the very best functional outcome from this surgery.
BEARING SURFACES
Wear of the bearing surface is the main cause of failure of hip replacements. Wear of the hip produces microscopic particles and these particles induce bone loss (osteolysis) and loosening of the components.
To address this problem alternative bearing surfaces have been developed. The benefits and disadvantages of each bearing surface are matched to patient profile and the best combination is selected.
UHMWP (Polyethylene)
Traditional hip replacements used ultra high molecular weight polyethylene and cobalt chrome femoral heads. This combination remains successful for the older population but advances in the manufacture of UHMWP (cross linking) have improved its wear characteristics.
Ceramic
Ceramics are hard, smooth and well lubricated. They can be used in combination with UHWP or against a similar ceramic counter face. They have the lowest rate of wear but are expensive and have a small risk of fracture or squeaking.
Metal
Metal on metal hip replacements are no longer used due to high production metal particles. Metal femoral heads are still very successful in combination with UHMPW.
ACTIVITY AFTER HIP REPLACEMENT
Walking and activity is vital for the optimum result after surgery and after all - what is the point of surgery if you don't use your new joint? However impact sport is likely to be detrimental.
If you require any invasive procedures following joint replacement - particularly dental work or bowel surgery please inform your treating professional about your joint replacement as you may need antibiotics to protect your joint replacement from infection.